Menopause and hypermobility can be a challenging duo. Falling oestrogen can affect connective tissue, muscle support and recovery time, which may worsen joint pain and fatigue in women with hypermobility and Ehlers‑Danlos Syndrome (EDS). In this article, I explain how menopause and hypermobility interact, common symptoms, and how you can manage joint pain.
To understand more about menopause in general, you may find my Menopause Guide for Women Over 45 helpful.
What is hypermobility?
Hypermobility refers to joints that move beyond the normal range (imagine acrobats with their legs bent behind their heads). When this flexibility comes with pain and frequent joint injuries, it may signal an underlying connective tissue disorder such as Ehlers‑Danlos Syndrome (EDS). EDS is a group of genetic conditions that affect collagen, the protein that gives strength and elasticity to skin, ligaments, blood vessels and organs.
The most common form, Hypermobile EDS (hEDS) — the one I live with — is marked by unstable, easily dislocated joints, chronic pain, stretchy or fragile skin, digestive problems, easy bruising and often intense fatigue. Living with EDS means dealing with both visible and invisible symptoms that can affect every part of daily life.
How hormones affect hypermobile joints
As explained on the Menopause: Complete Guide for Women Over 45, menopause, with its hormonal swings, shakes up just about everything in the body. Lower oestrogen and progesterone levels can change how connective tissues and muscles behave, which may exacerbate symptoms for those who are hypermobile. Research and clinical experience suggest that joint pain, tendonitis, muscle aches, mood swings, sleep problems and fatigue can all feel more intense when hypermobility sits on top of the menopause transition (just when you thought it could not get any worse).
Some women notice increased joint laxity (that loose, unstable feeling), more sprains, vaginal dryness and worsening pelvic floor dysfunction. Hormonal changes can influence connective tissue and pelvic support, so menopause and hypermobility can feed off each other and amplify symptoms.
Digestive symptoms when menopause and hypermobility collide
Hypermobility doesn’t stop at the joints. The same loose connective tissue can affect the digestive tract, leading to multiple symptoms:
- Acid reflux (heartburn)
- Bloating and abdominal discomfort
- Delayed gastric emptying and constipation
- Food intolerances
- Difficulty with bowel movements
- IBS
- Pelvic organ prolapse
All this overlaps with menopause, which can also slow down digestion, increase bloating, and make IBS symptoms worse.
When symptoms cross over
There are times when the pain, stiffness, and fatigue are worse than ever. Menopause may increase joint pain, while hypermobility makes healing slower and injuries more common. Tracking symptoms can help—writing in a journal or using a symptom tracker. For hypermobile women, healing often lags behind expectations and rest periods may need adjusting.
Tips To Manage Menopause‑Related Joint Pain When You’re Hypermobile
Hypermobile pain during menopause may call for using different strategies:
- Heat packs or warm showers/baths for soothing tense muscles
- Gentle stretching or restorative yoga to support joints and ease soreness
- Meditation or mindfulness to help with anxiety and stress, which can flare up pain
- Splinting or bracing: wearing joint supports during exercise or daily tasks to prevent overextending and limit injury risk
- Swimming smart: shorter, regular sessions, as swimming is often beneficial but can also trigger tendinitis in hypermobile joints
Key supplements and nutrients
- Magnesium: Supports muscle relaxation, eases cramps, and may help sleep and anxiety
- Vitamin C: Critical for collagen synthesis and joint healing; consider both foods (citrus, broccoli) and supplements
- Turmeric: Natural anti-inflammatory for arthritis and joint pain
- Rose hips and stinging nettle: Rich in antioxidants and plant compounds that support collagen and reduce inflammation
- Omega–3 fatty acids: Found in chia, flaxseed, walnuts, and fatty fish or supplements. They are natural anti-inflammatories; useful for pain and menopausal symptoms
Remember that dosing and interactions should always be checked with a doctor/GP.
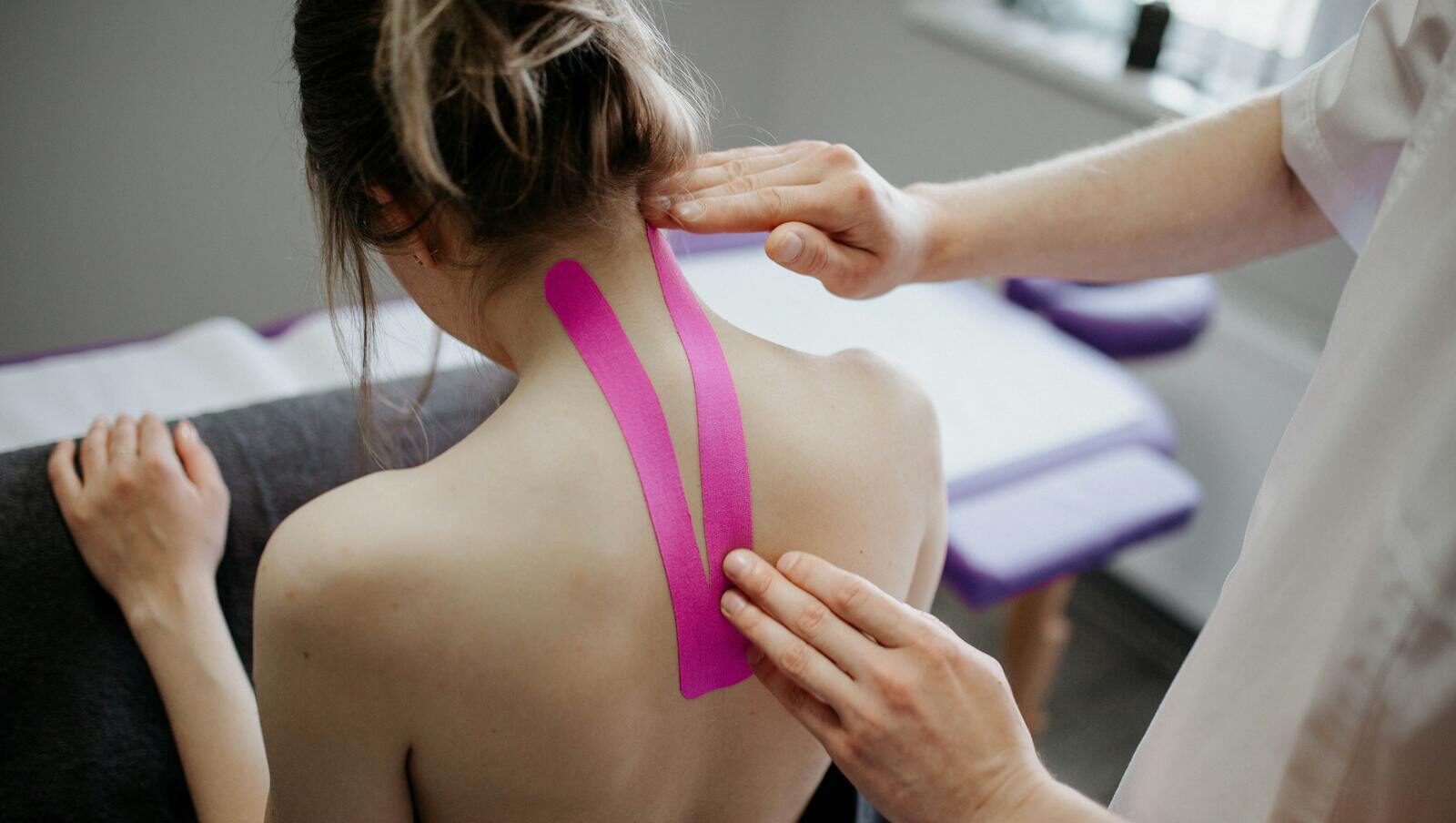
 Photo by Yan Krukau/Pexels.com
Photo by Yan Krukau/Pexels.com
Healing foods
- Leafy greens: Rich in magnesium, vitamins, and anti-inflammatory compounds
- Nuts and seeds: Almonds, cashews, pumpkin seeds
- Whole grains: Quinoa, brown rice for added fiber
- Fiber-rich foods: Whole grains, legumes, veggies help digestion and bowel health
- Limit sugar and processed foods: These worsen inflammation and digestive troubles
- Adequate hydration: Water, herbal teas (ashwagandha, black cohosh may help some menopause symptoms but always consult your doctor for dosing).
Managing insulin resistance and weight
Menopause aggravates insulin resistance — a real challenge for weight management. Lower estrogen, increased abdominal fat, disrupted sleep, stress, and reduced physical activity are all drivers. Here’s what helps:
- Focus on low glycemic load foods: whole grains, legumes, non-starchy vegetables
- Strength training: helps with muscle mass, mobility, and insulin sensitivity
- Cardio, like walking or cycling: useful for overall metabolic health
- Small, frequent meals: can help manage blood sugar spikes
- Stress management: meditation and deep breathing to reduce cortisol spikes
Living with menopause and hypermobility day to day
- Be gentle with your body: Healing takes longer, setbacks happen
- Track your symptoms: Journals help separate menopause from hypermobility
- Rest and pace yourself: Embrace good days, respect the bad ones
- Prioritise mental health: Anxiety and low mood can be overwhelming — don’t hesitate to seek help
- Celebrate small wins: Each swim, every walk, each joint that feels a little steadier matters to your long-term wellbeing
My experience
Looking back ten years, life with EDS already meant I had to pace myself — if I felt tired or achy, I’d stop, rest for a few days, and usually bounce back enough to get on with things. These days, menopause is like a tricky guest that moved right in, bringing lots of new challenges along for the ride. Suddenly, there’s a whole bunch of changes to deal with and it can feel overwhelming. The worst is insulin resistance; now, no matter how sensibly I eat or how much I want to lose weight, the scale refuses to budge.
Swimming is the only thing gentle enough for my joints, and when I finally manage to build a routine — motivated, determined to swim three times a week — something else goes wrong. My hypermobile shoulders can’t take the repetitive action, and sure enough, I end up with tendinitis in my left one. Last year it was my knees and tailbone—so painful I couldn’t walk or even sit. It was, to put it mildly, an interesting time. Sometimes I feel like I’m being penalised just for trying to look after myself and be healthy — and, heaven forbid, actually lose a bit of weight.
It’s an endless, frustrating cycle. When pain or fatigue hits, I wonder: is this menopause, or my bendy collagen acting up? The truth is, it’s both — menopause is making my hypermobility symptoms more intense, while hypermobility is feeding into my menopause struggles. It can feel like a never-ending tug-of-war, with no clear winner. But even when it seems impossible, I remind myself that resting, and not giving up are the only way forward. And if sharing how tough it can be helps someone else feel less alone, then at least the battle isn’t for nothing.
And in a couple of weeks I’ll be back in the pool again!
Have you had similar experiences living with menopause and hypermobility? If you have any stories, tips, or questions, I’d love to hear from you. Share your thoughts in the comments!
Frequently Asked Questions
1. Can menopause make hypermobility joint pain worse?
Yes, many women with hypermobility or Ehlers‑Danlos Syndrome (EDS) notice their joint pain gets worse in perimenopause and menopause. Falling oestrogen can affect collagen, connective tissue and inflammation, which may increase pain and reduce stability in already flexible joints .
2. Is joint pain in menopause always caused by hypermobility?
No. Joint pain in menopause is common even in women without hypermobility, and can be related to hormonal changes, osteoarthritis, weight changes, activity levels or other conditions. If you’re hypermobile, menopause can add an extra layer, so it’s important to talk to a healthcare professional to rule out other causes and get a proper assessment .
3. What gentle exercises are safest if I’m hypermobile and in menopause?
Generally, low‑impact, controlled movement is safest: options like swimming, Pilates, yoga with a focus on stability (not deep stretching), and light strength training to support muscles around your joints. Because hypermobility and menopause affect each woman differently, it’s best to work with a physiotherapist or trainer who understands both joint instability and midlife hormonal changes.
Disclaimer: Always consult with your GP/rheumatologist/menopause specialist if you recognise yourself in the article. Silverlocks is supportive information, not a replacement for care.
References
- Linda Andersen – Doctoral Dissertation, University of Missouri, 2023 – Health related quality of life in midlife and older women with Hypermobile Ehlers-Danlos Syndrome
- Hypermobility.org – Types of Hypermobility
- National Library of Medicine – Hypermobility and Chronic Pain
Read more on Silverlocks
- Why does turning 50 feel so scary for some women?
- Perimenopause x Menopause: what is the difference?
- Menopause and mental health: how to calm anxiety and lift your mood naturally