If you feel like you’re doing everything “by the book” and still gaining weight—or not losing a single kilo—please know you’re not going crazy and you’re definitely not alone. In this article, I want to walk you through the hidden link between menopause and insulin resistance, how thyroid issues can make it worse, and what real‑life changes can help us regain at least some control over our bodies again. For more information about other symptoms check the Menopause Guide.
The hidden link between menopause and insulin resistance – in plain language
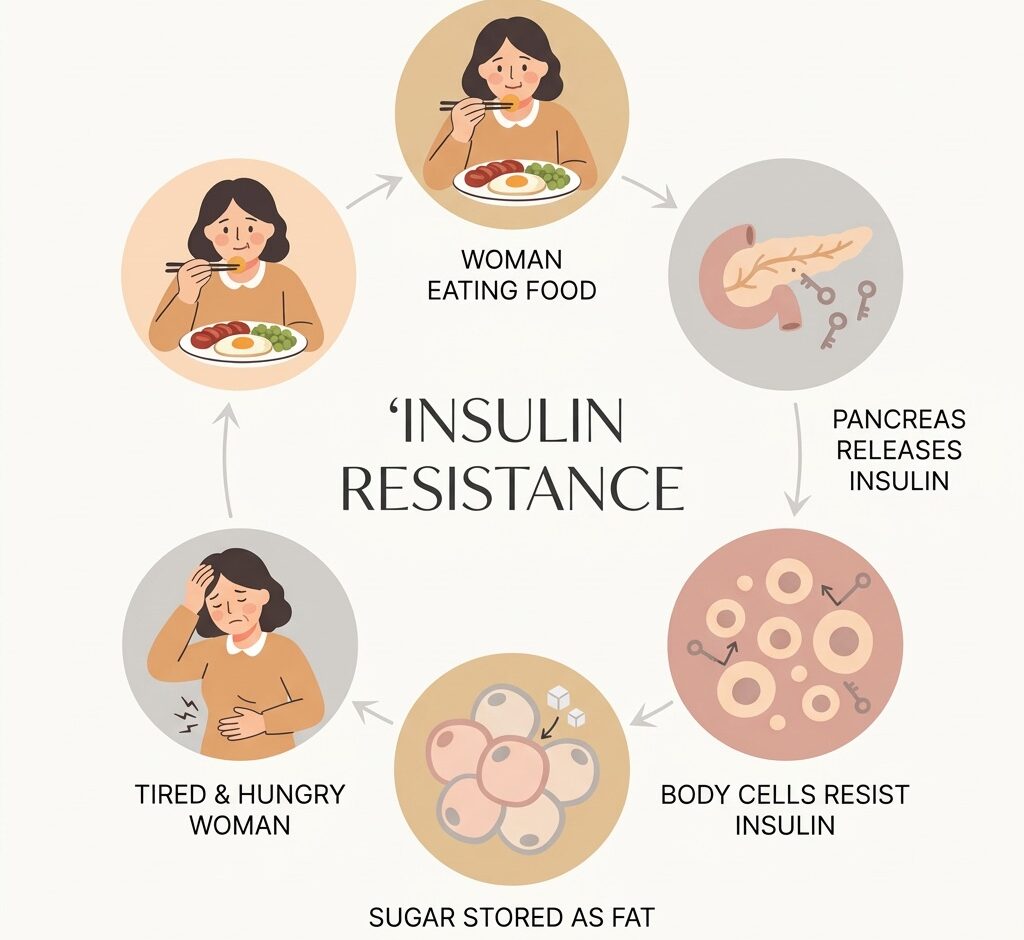
Insulin is a hormone made by your pancreas that acts like a key. When you eat, food is broken down into sugar (glucose), which travels in your blood. Insulin “knocks” on your cells and tells them, “Open up, let the sugar in so we can use it for energy.” When everything works well, your body makes a small amount of insulin, the doors open, sugar goes in, and your blood sugar stays in a healthy range.
With insulin resistance, those doors don’t respond properly anymore. The locks become “rusty.” Your body still makes insulin (often more than before), but your cells ignore it, so the doors only open halfway. That means more sugar stays in your blood. Your pancreas keeps pumping out more and more insulin to try to fix the problem. The extra insulin tells your body, “Store, store, store,” especially around the abdomen.
Over time, this constant high‑insulin state doesn’t just affect weight. It also puts more fat around your organs (visceral fat), which is strongly linked to heart disease and metabolic problems. Can raise triglycerides, lower “good” HDL cholesterol, and increase blood pressure as part of metabolic syndrome. Makes you more tired after meals and more likely to crave carbs and sweets, because your cells still feel “hungry” even when your blood sugar is high.
The annoying part? Insulin resistance is often silent for years. You can have “normal” fasting glucose. A1c that is still not in the diabetic range. But insulin levels that are already high and a body that is already struggling.
If nothing changes, this long, quiet phase can slowly turn into pre-diabetes and, later, type 2 diabetes. That’s why so many experts now talk about insulin resistance and pre-diabetes as a wake‑up call rather than something to ignore.
Menopause and Insulin Resistance: Why menopause makes insulin resistance worse
Menopause doesn’t “create” insulin resistance out of nowhere, but it certainly doesn’t help. Falling oestrogen changes where we store fat and how our bodies handle sugar and insulin.
Research shows that after menopause, we tend to store more fat around the waist and organs instead of hips and thighs. This visceral fat is very active tissue—it releases inflammatory substances that push the body further toward insulin resistance and unhealthy cholesterol patterns. Even women who were always a stable size can gain about half a kilo a year in midlife, especially around the middle.
On top of that, sleep and stress often get worse. Night sweats, joint pain, and anxiety can disturb sleep, and poor sleep itself makes insulin resistance and appetite worse. Chronic stress raises cortisol, which loves to “help” you store fat around the belly.
So if you feel like the rules changed overnight in your late 40s or 50s, they did. Your hormonal background has shifted, your body composition is changing, and insulin resistance fits right into that picture for many women.
Hypothyroidism, menopause and insulin resistance
As if menopause weren’t enough, thyroid issues often join the party. Hypothyroidism (an under active thyroid) slows down metabolism and can promote weight gain and higher cholesterol. Studies suggest low thyroid hormone levels can be linked with more insulin resistance, and this association may be stronger in postmenopausal women.
In real life, this means that you may be dealing with low oestrogen, sluggish thyroid, and insulin resistance at the same time. You’re tired, your muscles feel weaker, and the scale barely moves, even when you are trying.
If this sounds familiar, it’s not “too much drama”—it’s a real combination many women over 50 are living with. A good endocrinologist can help you look at all these pieces together, not just one lab number at a time.
Menopause and Insulin Resistance: why you gain weight even when you’re careful
Many midlife women say the same thing: “I move more and eat less than ever, and yet nothing changes.” Here’s why that can happen with insulin resistance and menopause:
- Your old “maintenance” lifestyle is no longer maintenance. The same food and activity that kept you stable at 35 may maintain a heavier weight at 55 because of hormonal and metabolic changes.
- High insulin is a strong storage signal. When insulin is high, your body protects fat stores instead of using them, especially around the waist.
- Less muscle means less burning power. We naturally lose muscle after 40–50, especially if we’re not doing strength work. Less muscle means lower metabolism and less room to “park” glucose in a healthy way.
- Poor sleep and stress quietly sabotage your efforts. Both push your body toward higher blood sugar, more cravings, and more belly fat.
So no, you’re not weak or lazy. You’re rowing upstream in a different river than you were 20 years ago.
Menopause and Insulin Resistance: what actually helps
The good news: you don’t need perfection or extreme diets. But you do need consistency and some midlife‑specific tweaks. Studies show that lifestyle changes—especially around food quality, movement, and weight—can improve insulin sensitivity and delay or prevent diabetes.
A few pillars that really matter:
- Carbs: focus on quality and combinations
Choose slow, fiber‑rich carbs (beans, lentils, oats, barley, quinoa, whole grains, fruit, vegetables) and go easy on refined white carbs and sugary foods. Pair carbs with protein and healthy fats so your blood sugar rises more gently. - Protein and fiber: non‑negotiables after 50
Protein helps maintain muscle and keeps you fuller; fiber slows down sugar absorption and supports your gut. Aim for a protein source at each meal and plenty of plants (veg, fruit, legumes, nuts, seeds, whole grains). - Movement: don’t just move, build
Cardio (like walking or swimming) is fantastic, but adding 2–3 short strength sessions per week makes a big difference to muscle and insulin sensitivity. This can be as simple as body‑weight exercises or light weights at home. - Sleep and stress: they’re not “extra”
Protecting your sleep and giving your nervous system small breaks during the day is part of treatment, not a luxury. Even simple routines—a calming bedtime ritual, 10‑minute walks, breathing exercises—can support your hormones.
And yes, for some of us, lifestyle changes alone are not enough. Medications like metformin or GLP‑1 agonists may be added by doctors to help reduce insulin resistance and diabetes risk in high‑risk women.
Menopause and Insulin Resistance: my experience
I’ve been living with insulin resistance for some years now, and for a long time I didn’t even know it had a name. All I knew was that no matter how much I exercised or how carefully I ate, the weight simply refused to move.
Because I also have hypothyroidism, once a year I see my endocrinologist and have blood test done. About three years ago, during one of those routine check‑ups, she looked at my results and told me the news: insulin resistance had joined the list.
To be fair, maybe I had a tendency to develop it anyway. It runs in many families, and midlife weight changes are common. But I’m pretty sure menopause gave it a little “push,” let’s say it like that. My endocrinologist first prescribed Saxenda. I used it for a couple of months, it helped for a while, but once I stopped, the weight slowly crept back on—very typical with this kind of medication if the underlying habits and hormones are still there.
Now I’m on another medicine to help with insulin resistance, I’m trying to keep up with exercise, and I focus a lot on lean protein (I’m pescatarian) and increasing my fiber intake. It’s not perfect, but it’s a more realistic way for me to live with this body instead of constantly fighting it.
After I started going through menopause, I came to a funny—but true—conclusion: menopause symptoms plus being over 50 is a bit like being a baby again. You’re suddenly “not allowed” a lot of foods, you have to count how much you eat (especially protein and fiber), and your body has very strong opinions about what it likes and what it doesn’t. The bliss of being an older woman, right?
So if you’re in the same boat—juggling menopause and insulin resistance, weight that won’t budge, and a body that doesn’t feel like your own anymore—please know you are not alone.
Share your experience in the comments. Let’s help each other, compare notes, and remind ourselves that our worth is not measured in kilos, sizes, or blood sugar numbers.
Disclaimer: This article is for information and support only and is not a substitute for personal medical advice, diagnosis or treatment. Always talk to your GP, endocrinologist or other qualified health professional about your own symptoms, test results and medications, especially if you have diabetes, pre-diabetes, thyroid disease or are taking drugs that affect blood sugar. Never ignore or delay seeking professional advice because of something you have read on Silverlocks.
References
- Grem Journal – Metabolic syndrome, insulin resistance and menopause
- National Library of Medicine – Insulin Resistance
- CDC – Insulin Resistance and Type 2 Diabetes
- Mayo Clinic – The reality of menopause weight gain